Blog · Sleep Position
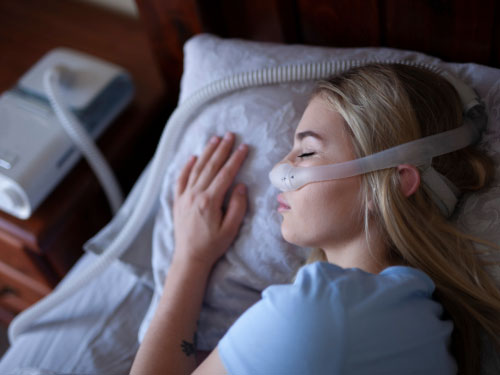
The short answer
The single best sleeping position for the majority of snorers and sleep apnoea patients is on the side — specifically the recovery position, where the face is angled slightly downward and the chin sits a little forward. Stomach sleeping comes a distant second. Back sleeping is the worst.
In an audit I ran of 6,044 NHS patients with diagnosed obstructive sleep apnoea:
- 60.3% no longer met the clinical threshold for sleep apnoea when sleeping on their side
- 85.7% showed at least a 20% improvement in OSA severity
For most people, the right position is a more powerful intervention than anything I can prescribe in clinic. It is free. It has no side-effects. It requires no surgery, no device, no medication. And the data say it works in around six patients out of ten.
The catch is consistency. Trying side sleeping for one night, drifting back onto your back at 3am, and concluding that "it didn't help" is the most common mistake. The benefit comes from staying on the side, all night, for long enough that the body adapts. That usually means three things: a pillow tall enough to make the position comfortable, something to physically discourage rolling onto the back, and two to three weeks of consistency before you judge whether it has worked.
Why position matters so much
The throat is a soft, collapsible tube. Unlike the windpipe lower down, it has no rigid cartilage to hold it open. It stays open during the day because the muscles of the tongue, palate and pharynx are actively keeping it open. The moment you fall asleep, those muscles relax. Whether the airway then stays open or collapses comes down almost entirely to two things: how much spare room there is in the throat, and which direction gravity is pulling the tongue and soft palate.
When you sleep on your back, gravity pulls the tongue and soft palate backwards into that tube and partially blocks it. Air still gets through — but only by vibrating the tissue. That vibration is what we call snoring. If the airway closes completely for ten seconds or more, that's an apnoea. If it narrows enough to make breathing genuinely hard work without fully closing, that's Upper Airway Resistance Syndrome (UARS) — a third category that is just as exhausting as apnoea and often missed entirely on standard sleep studies.
Turn onto your side and gravity now pulls the tongue and palate forward, away from the airway. The throat stays open. Snoring quietens. Apnoeas reduce. The respiratory effort needed to move air falls. The body stops paying a sympathetic-nervous-system price for breathing. In the recovery position the effect is even stronger because the face is tilted slightly downward — the optimal angle for keeping the airway clear and letting any secretions drain forward out of the throat instead of pooling at the back of it.
Endoscopic sleep studies — where we watch the airway with a small camera while the patient is sedated into a sleep-like state, a procedure called DISE — make this visible. Turn the patient onto their back and the airway collapses dramatically; rotate them onto their side and, in most cases, the airway reopens in real time. It is not a subtle effect. It is one of the most striking things you can watch in a sleep laboratory.
Ranking the positions
1. Side, in the recovery position — best
Face slightly downward, chin a little forward, top knee bent and resting forward of the lower knee. This is the position the body naturally finds when fully relaxed on the side. It maximises airway opening and reduces both snoring and apnoeas more than any other position.
2. Straight side sleeping — good
Face level rather than angled down. Better than back sleeping but doesn't gain the full benefit of the recovery angle.
3. Stomach (prone) — reduces snoring, loads the spine
Stomach sleeping is genuinely effective for snoring because the head tends to turn to one side and the airway clears. The problem is the neck rotation and lower-back arch, which create musculoskeletal issues over time. Stomach sleeping also makes acid reflux worse for some people.
4. Back (supine) — worst
Maximum airway collapse. The tongue, soft palate and even the epiglottis all fall back under gravity. Snoring is loudest, apnoeas are deepest, oxygen drops are largest, and arousal frequency is highest. If you have any tendency to snore or apnoea, this is the position that brings it out — and many people who consider themselves "non-snorers" snore the moment they end up on their back after a glass of wine or with a cold.
What the evidence shows
Side sleeping is not a fringe recommendation. The body of literature now extends well past my own audit:
- Around 50–60% of people diagnosed with OSA have positional apnoea — defined as at least twice as many events on the back as on the side.
- Randomised trials of positional therapy (devices that prevent supine sleep) show consistent reductions in apnoea index, snoring loudness, and daytime sleepiness.
- Patients on CPAP frequently need lower pressures when they sleep on their side, with corresponding improvements in mask comfort and adherence.
- In hypoglossal nerve stimulator (Inspire / Genio / Restera) responders, side sleeping produces additive improvement over the implant alone.
For a treatment that costs nothing and has no side-effects, that is an extraordinary evidence base.
Snoring vs sleep apnoea — does position help both?
Yes. The mechanism is the same. Snoring is the sound of partial airway vibration; apnoea is the consequence of complete airway closure; UARS is a sustained, effortful narrowing without complete closure. All three improve when gravity is removed from the equation by sleeping on the side.
The biggest gain tends to be for patients with mild-to-moderate OSA, simple snoring, or UARS. Severe OSA usually benefits but rarely returns to a normal AHI on position alone — these patients typically need CPAP, an implant or surgery in addition. Position is then a complementary strategy that lowers the dose of the primary treatment.
How to actually stay on your side
If side sleeping were easy, everyone would already be doing it. The challenge isn't intent — it's that ordinary pillows make side sleeping uncomfortable, so the body drifts back to its old position within an hour or two.
The trick is removing the discomfort that drives you back. That means:
- A head pillow that supports the neck at the right height for side sleeping (usually taller than what most people own)
- Some physical resistance — usually a body pillow or wedge — to stop you rolling onto your back during deep sleep
- 2–3 weeks of consistency before the new position becomes the default
This was the reason I designed the Side Sleep Pro two-piece system and the Dual Comfort Pro head pillow — most patients giving up on side sleeping were doing so because of pillow discomfort, not because the position itself wasn't working.
Read further
The full version of this article — with deeper detail on the published evidence, sleep-stage data, and the practical adjustment protocol — lives on the I Want Great Sleep blog.
Read the full article →What if I have CPAP, an implant, or other treatment?
Side sleeping complements all of them. CPAP works at lower pressure when the airway is already mechanically open — which means a better night, less mask leak, and easier adaptation. Hypoglossal nerve stimulator (Inspire / Genio / Restera) patients tend to get a stronger response on their side. After surgery, side sleeping reduces tissue swelling at the back of the throat and helps recovery.
The honest caveats
About 15% of OSA patients are not positional — their apnoea is similar regardless of how they lie. If you've genuinely committed to side sleeping for a month and your symptoms haven't shifted, that's important information and worth investigating. The next step is usually a proper sleep study to characterise the apnoea pattern, followed by a structured assessment of where the airway is actually collapsing.
There is a second group worth flagging here. Some patients sleep faithfully on their side, snore much less — and still wake up exhausted. The conventional sleep study often comes back normal because there are no apnoeas to count. This is the territory of Upper Airway Resistance Syndrome, where the airway is narrow enough to make breathing effortful all night without ever fully closing. We have built a dedicated re-analysis service for exactly this pattern, using new metrics — Ventilatory Burden, Thoracoabdominal Asynchrony Burden and Autonomic Burden — that pick up the effort and stress the standard AHI ignores. If you tick that box, position alone will not be enough, and you deserve a more sensitive assessment.
Shoulder pain, hip pain, certain pregnancy-related conditions, and recent shoulder surgery can all make side sleeping temporarily uncomfortable. The fix is usually the right pillow and a knee pillow, not abandoning the position — but seek medical advice if you are recovering from an injury or operation.
Common questions
Left side or right side — does it matter?
For airway physiology, no — either side is dramatically better than supine. There are some small differences in other systems: left-side sleeping reduces acid reflux (the gastro-oesophageal junction sits higher than the stomach) and improves cardiac output in heart-failure patients; right-side sleeping is often more comfortable for healthy adults. Pick whichever side you prefer and don't worry about the rest.
What about my CPAP mask — does side sleeping help or hurt?
Helps, on balance. Side sleeping reduces the pressure the machine needs to deliver, which usually means less mask leak, less aerophagia, and better tolerance. The mask itself may need adjustment for side sleeping — a smaller nasal pillow or a low-profile full-face mask works best — but the gain in physiology is worth the small kit change.
Will I ruin my shoulders by sleeping on my side?
Not if the head pillow is the right height. Most shoulder pain in side sleepers is the result of an under-tall pillow forcing the head to drop and the shoulder to bear the weight. A pillow that fully fills the gap between the side of the head and the mattress eliminates the problem.
Try it for two weeks
If you take one thing from this article: spend the next two weeks deliberately starting every night on your side, in the recovery position, with the best pillow you have available. Ask your partner (or use a recording app) whether your snoring has changed. Track your sleep with a wearable if you have one. Most people are surprised by the result.